Help and hope for moms: earlier mental health screening and support
Posted on November 23, 2021
For some people, the experience of pregnancy and transition to motherhood is coloured by severe depression and/or anxiety, and further complicated by limited access to mental health supports when they need it. When left untreated, these issues can become pervasive in a person’s life.
Improving access to mental health supports in the limited time period before and after delivery is the inspiration behind a Shared Care perinatal mental health project - a physician-led collaboration that aims to help an estimated 1000-plus people living in Southern Vancouver Island.
Identifying issues earlier
Victoria-based family physician Dr. Alicia Power recognized that earlier screening and treatment of mental health issues was needed to support the well-being and health outcomes of patients.
As many as 16% of people experience significant depression at some point during their pregnancy and up to 31% experience major depressive disorder during the first year postpartum.
Identifying gaps and exploring solutions
In 2019 Dr. Power collaborated with three family physicians, a midwife, a psychiatrist, and two public health nurses, as part of the Shared Care South Island Perinatal Mental Health project, to tackle the problem.
Their approach included the engagement of maternity care providers from across the spectrum to define the scope of the issue, identify gaps, and explore options and solutions.
The group successfully implemented improvements, working swiftly to make changes in three key areas:
-
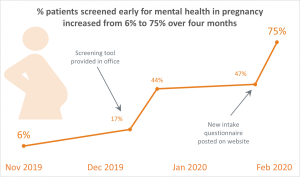
Increased mental health screening early in pregnancy: Standard screening for all perinatal patients in the first trimester increased from 6 per cent to 75 per cent in just four months between November 2019 and March 2020 in the Grow Health Clinic where Dr Power and other physicians see about 700 patients each year. The team further hosted a learning event to encourage other clinics to also adopt standard screening. Additionally, an information poster was created to help patients in early pregnancy feel comfortable talking about their mental health.
-
Awareness of Perinatal Mental Health resources: A list of clinics, public health resources, counselling, support groups, online reading, books, podcasts and videos was created and made available to providers and patients.
-
Access to outpatient perinatal psychiatry services: Collaboration has fast-tracked access for perinatal patients to a cognitive behavioral therapy (CBT) skills group. Additional providers and specialists from pediatrics, midwifery and family practice were further engaged to work on medication support, provider education, and a peer support program.
The group’s accomplishments in these areas inspired them to take the project to the next level. This involves creating a broader ‘umbrella’ perinatal mental health group to support the mental well-being of families from pre-conception to early childhood years.
New relationships key to success
The success of the Perinatal Mental Health Project was undoubtedly fueled by the excitement and passion of participants working with multi-disciplinary teams on meaningful, tangible solutions. One participant commented, “A big benefit of the project was the relationships that were developed throughout the team that were not there to begin with.”
“This project allowed all of the players in perinatal mental health in Victoria to come together and create collaborations, and to understand how to best use local resources and improve current systems for pregnant people needing mental health care in Victoria.” says Dr. Power.
Ongoing Benefits
Dr Power speaks to the legacies of the project: “A few important initiatives were spawned and are ongoing from this work to improve our system. We have improved screening and access to all aspects of care through this work, and as a community are continuing to work more collaboratively to support this high-risk population.”
THE TEAM
Family Physician (FP) Lead: Dr Alicia Power
Specialist/GP Focused Practice Leads: Dr. Joanna Cheek (Psychiatry), Dr Jasmina Kobiljski (Perinatal Psychiatry), Dr. Bryony Corbin, (Perinatal Psychiatry)
Other providers: Tracy McGee (Clinical Counsellor), Emma Jackson (FP resident), Lauren McHattie (Midwife), Kathy Easton (Public Health), Dianna Dall’Aqua (Public Health), Dr. Shana Johnston (FP), Dr. Laura Birdsell (FP)